One October morning a little after 6 a.m., a yellow Mercedes-Benz weighed down with thousands of pounds of explosives drove through the five foot-high barrier of concertina wire surrounding the Beirut International Airport. This rather large facility was where the United States Multinational Force was headquartered, providing shelter to more than 350 military personnel. As the truck bypassed soldiers on watch, it continued to gain speed, plowing through a guard shack, and penetrating the Battalion Landing Team Headquarters building before detonating.
In a matter of seconds, the structure collapsed to rubble, killing 234 people instantly. The explosion was so powerful, it’s believed that it could have occurred 330 feet from the building and still produced major structural damage and caused significant casualties.
As survivors began to dig through the dust and debris with their bare hands, the mass casualty plan was set into motion. Assistance from Britain, France and Israel were offered almost immediately. Triage and treatment sites were set up, medical support units were transported to the scene, evacuation aircrafts were requested. Victims that could be identified after being pulled from the debris, were. Due to the sheer catastrophic nature of the explosion, some seriously wounded patients were delayed approximately four hours before arriving at hospital facilities.
It was with this situation that the Department of Defense Commission began to explore fundamental changes in improving medical care in support of combat operations.
All of life is a matter of timing.
For Stephen Barnes, MD, FACS and chief of the Division of Acute Care Surgery at University of Missouri Health Care, the interest in trauma care synced up with the shift in the political and global landscape following the terrorist attacks on the United States, Sept. 11, 2001. Taking part in the Health Professions Scholarship Program, a United States Air Force scholarship offering, Barnes graduated from the University of Alabama School of Medicine. He was then put on inactive reserve status by the Air Force to undergo further training in general surgery, trauma and critical care for seven years until he found himself stationed in Cincinnati, Ohio.
Early on in conflict the Department of Defense identified that military hospitals were not trauma centers, as they provided care to a mainly healthy and aging population. In order to provide pre-deployment trauma training to active duty guard and reservists, the Department of Defense set up a number of joint civilian-military training programs across the United States, including one in conjunction with the University of Cincinnati Medical Center, known as Centers for Sustainment of Trauma and Readiness Skills (C-STARS).
“We were there for individuals who sacrificed in support of our country,” Barnes says. “It was a very easy patient population to take care of.”
So, as the timing would have it, Barnes would begin his active duty status as a major in the United States Air Force — at a civilian hospital in the southwest corner of Ohio.
“As a trauma surgeon, it was great,” Barnes explains. “At the time, the Air Force only had one trauma center, in San Antonio, so this allowed me to leave fellowship and do the two things professionally that I like to do the most, which is teach and take care of the severely ill and injured.”
Barnes, and other active duty Air Force members at C-STARS in Cincinnati, were deployed in multiple teams in support of Operation Iraqi Freedom and Operation Enduring Freedom to Iraq and Afghanistan in order to remain current on learnings from the field. The goal was to bring back lessons learned to the C-STARS training program so that they were teaching and training in real time.
Many lessons are learned with the onslaught of battlefield injuries in a time of combat. Historically, monumental changes have been made in the way injury care is delivered, due simply to the fact that on the frontlines of conflict, a large volume of severe injuries occur in a short period of time. In the first Gulf War, though the number of casualties was few, the case fatality rate — the proportion of deaths over a defined period of time — was high. This, in part, could be attributed to bringing a Vietnam era medical stance to a combat setting in the early 1990s, nearly 20 years after the Vietnam War had ended.
The challenge of providing medical care in a combat setting is three-fold, according to Barnes.
Challenge #1 | How do you provide medical care in a combat zone?
During the Gulf War, combat medicine was “in the rear with the gear.” The Air Force hospital that supported the operation was located on an old air field in Egypt, far removed from the conflict where soldiers were being wounded in Iraq. In an effort to make an impact on preventable causes of death, combat medicine moved away from the “rear with the gear” mentality in order to create lightweight, lean and mobile capabilities to put adequate care within a meaningful distance of the injured.
Because of this shift in moving medical care closer to point of wounding during the Gulf War, modern warfare survival rates in subsequent times of conflict improved greatly — sometimes reaching a 97 percent survival rate as seen in Balad during Operation Iraqi Freedom.
Challenge #2 | How are the critically injured safely transported to their next point of care?
With the implementation of forward surgical teams, surgeons were able to perform damage control surgery during combat within the “golden hour” of injury — a time period lasting for one hour, or less, following traumatic injury. Wounded warriors were then prepared for medical evacuation to a higher level of care through medical ground and air transport.
During the Vietnam War, the average injured soldier took 42 days from day of wounding to arrive in definitive care in the United States. By comparison, today, that timeframe is three to five days, taking into account the day of injury in Iraq or Afghanistan, a stop in Germany at Landstuhl Regional Medical Center for most patients, and then onto the most appropriate Department of Defense medical facility in the United States based on injury type.
“We were there for individuals who sacrificed in support of our country,” Barnes says. “It was a very easy patient population to take care of.”
Challenge #3 | How do you maintain a level of intensity within acute care coupled with rapid patient movement?
Damage control is the name of the game in post-combat casualty care. Named after the Naval process of sealing up a ship and controlling where the water goes in order to keep a ship afloat, the goal in combat is to stop the bleeding and major contamination during the first operation prior to performing any other surgeries. With an intense, staged approach to trauma care in combat, the life and limb saving surgeries may be separated by a helicopter flight, or even a transcontinental flight, to the next point of care. Staged care is all about providing a good foundation for the next surgeon to build on when conditions are less dangerous and are more controlled.
___
“The only people who gain from warfare are young surgeons,” said the 16th century French military surgeon Ambrose Paré, and for Barnes, that sentiment couldn’t be more accurate. Being a brand new trauma surgeon during a time of active military combat provided unparallelled learning opportunities.
“I was learning at a pace that couldn’t be achieved anywhere in the United States,” Barnes explains. “It accelerated my understanding and allowed me to teach others what I had learned.”
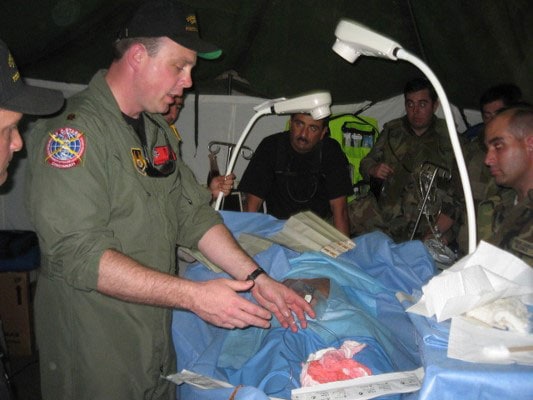
In 2006, Barnes left his very pregnant wife and three small children and deployed as a major in the United States Air Force. Each day, he walked through a series of tents on a plywood walkway, and into a converted cargo container to practice state-of-the-art trauma care for those he lovingly referred to as “America’s best.”
“We were there for individuals who sacrificed in support of our country,” Barnes says. “It was a very easy patient population to take care of.”
Despite the pride of providing care in a combat zone, many providing that care have to navigate between bouts of boredom and intermittent episodes of total fear and stress. But for Barnes, his location at Balad Air Force served as the exit point for all combat casualties. He was completely inundated with a continuous flow of wounded soldiers, far different than what he encountered at the university’s hospital in Cincinnati. He was used to seeing patients with single, sometimes multiple, low-velocity gunshot wounds. However, during his time in Iraq, he encountered patients with injuries sustained from IED explosions that presented with combinations of high-velocity, penetrating injuries, blunt trauma, blast and burn injuries. As a result, Barnes was forced to make decisions that have stuck with him.
“When the tempo was high, triaging mass casualty situations could be difficult because you have to make decisions based on the number of patients and number of resources.” Barnes explains. “I don’t miss that stuff. I like being in a fully resourced trauma center. I didn’t enjoy making those very hard triage decisions. But I’d go back tomorrow.”
When not formally deployed, Barnes focused on teaching and relationship building around the world to spread the knowledge he gained on the frontlines of combat.
“I was gone a lot,” Barnes explains. “I had the opportunity to travel throughout the world, teaching what we learned to other Americans and our allies, and improving other combat medical facilities. But the focus on the job was always the same — how do we best stop the bleeding and save lives.”
Providing care on the battlefield all comes down to timing. The timing of medical transport and the timing of surgical interventions all factored into the life or death outcomes of the wounded warriors, but before they can encounter transportation or surgery, the immediate threat has to be neutralized — stop the bleeding.
When looking at preventable causes of death, compressible hemorrhages with tourniquets was one lesson learned that carried over from the frontlines and into the operating rooms in hospitals all across the nation. When it came to an injury requiring a tourniquet, the mentality used to be “life over limb,” meaning that if a tourniquet was used on an injured soldier, that individual was going to lose their limb as a result, but likely go home with their life. Now, with research and implementation of better battlefield care, the choice between keeping your limb or losing your life doesn’t always have to be made.
As a result of definitive research by the Department of Defense, commitment, and training for those in the field, the use of the tourniquet was brought back into common practice. In current combat, all deployed personnel carry tourniquets that they can either apply themselves, or have applied by their fellow soldier, shifting the mentality that tourniquets could not only save lives, but could save limbs as well. But the usefulness of the tourniquet didn’t stop in the combat zone.
“I cannot think of an ambulance service in the state of Missouri that has not reintroduced the tourniquet into what our pre-hospital personnel utilize,” Barnes explains. “We utilize it in the operating room when needed and for immediate control of hemorrhage, and have seen higher survival rates and higher limb salvage rates when they’re applied early.”
In the battlefield, there are many injuries that require more attention. Junctional hemorrhages — bleeding from the areas at the junction of the trunk and its appendages — are one of those things, and remain the biggest killer on the battlefield. In 2001, the FDA rapidly approved multiple new procoagulant dressing products to be used in order to improve the odds of those suffering from junctional hemorrhages. Unlike traditional gauze, procoagulant dressings were effective at bringing the concentrated components needed to promote coagulation when tourniquets were inappropriate.
Despite the many improvements in combat medical care, vexing injuries like noncompressible hemorrhages, or bleeding in the chest or abdomen, keep physicians and researchers on their toes. Discussions at the Department of Defense on how to control noncompressible hemorrhages led to the development of the Resuscitative Endovascular Balloon Occlusion of the Aorta (REBOA) catheter.
“In the past, if we wanted to put a clamp on your major blood vessel that delivered oxygenated blood to your body in a hurry, we had to open your chest, reach in and place a clamp on your aorta,” Barnes explains. “With the development of this small, flexible, easy-to-place catheter, we can now access your groin and place the balloon in the same place in your chest, blow up a balloon to accomplish the same goal of rapid control of blood loss. This is significantly less traumatic to the patient.”
Under Barnes’ supervision, the University of Missouri Health Care’s Frank L. Mitchell Jr., MD, Trauma Center has implemented use of the REBOA catheter, providing yet another example of lessons learned in Iraq and Afghanistan that have been translated into civilian trauma care.
When teaching a multitude of people how to provide trauma care, Barnes was forced to rapidly learn, and subsequently teach, a curriculum that needed to evolve as best practice from the field also evolved. Much of that evolving knowledge has been applied to the way medical students, residents and fellows are taught at the University of Missouri — even finding its way into the “trauma Bible” used under Barnes.
“It’s a living book that changes almost quarterly as we learn better ways to provide care.”
“It’s a living book that changes almost quarterly as we learn better ways to provide care,” Barnes says. “We update and modify our practice management for trauma and acute care so that we don’t get stuck in that 50-year rut we were in from the 1960s to the early 2000s. We constantly reassess the way we both deliver care and educate others so that we’re always at the tip of the spear as a state-of-the art practice, rather than just using years of medical dogma to drive what we do.”
Though the location of his operating room has moved from the confines of a shipping container to the newly expanded emergency department and trauma bay, and the curriculum continues to evolve over the tenure of his career, his job has remained the same since the beginning — learn from death and destruction how to stop the bleeding and save lives.